Welcome To South Carolina Hip Preservation Center
South Carolina Joint Replacement Center | Midlands Orthopaedics recently merged with Columbia Neurosurgery to create Midlands Orthopaedics and Neurosurgery. Our goal is still the same: to provide cutting-edge treatments to patients with hip and knee pain.
Proudly Fellowship-Trained and Board Certified Orthopedic Surgeons Providing Expert
Surgical Care for
Hip Problems
-
Thomas P. Gross, MDBoard Certified & Fellowship Trained Orthopaedic Surgeon
Hip Resurfacing & Hip Replacement
-
Robert Browning, MDFellowship-Trained Orthopaedic Sports Medicine Surgeon
Hip Arthroscopy & Sports Medicine
-
0
17-year survivorship
for Hip Resurfacing -
0
18-year survivorship for Metal-on
-Metal Total Hip Replacement -
0
HRA Procedures
performed - 0
6-year survivorship revision
surgery for hip resurfacing
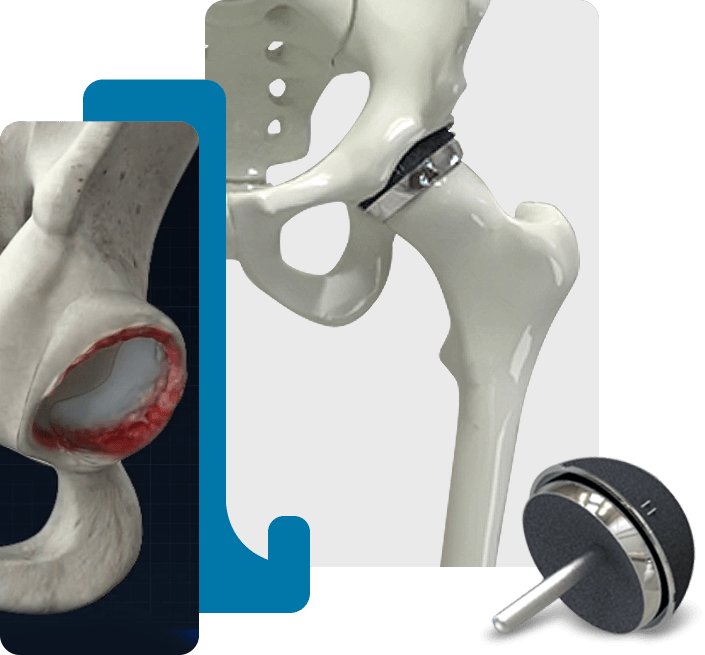
All About Hip ResurfacingWhy Choose
Hip Resurfacing?
Dr. Gross is one of only a few surgeons who performs total hip resurfacing. It's the best solution for near-normal reconstruction of the hip joint in severe arthritis. While complex to perform, it has the lowest failure rate of any type of hip reconstruction surgery.
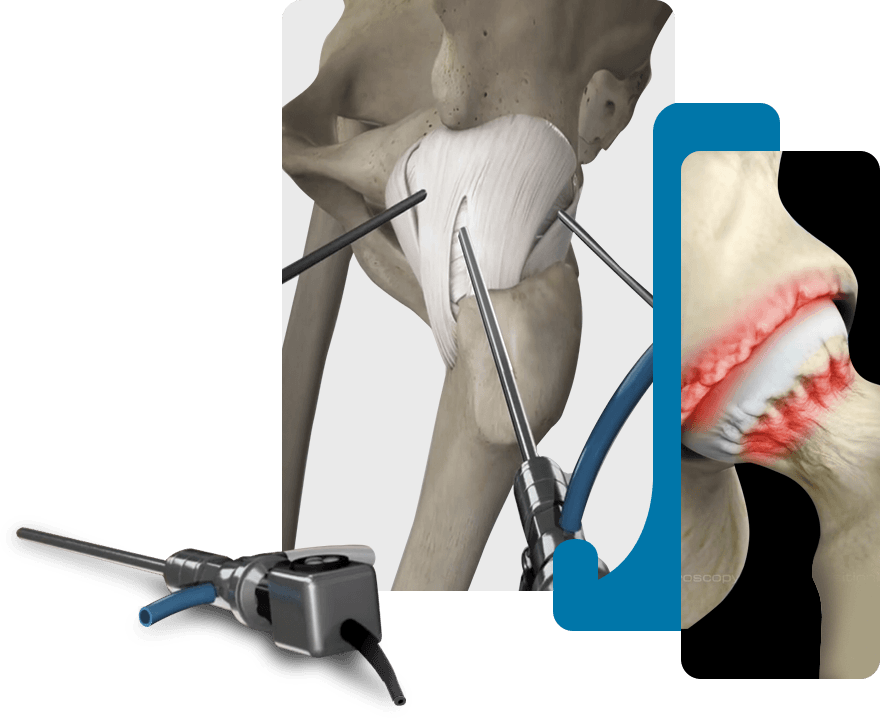
All About Hip ArthroscopyHip Arthroscopy for
Treatment of FAI
Hip arthroscopy is an available minimally invasive surgery for Femoroacetabular Impingement (FAI). The goal of the treatment is to decrease pain and increase function by reducing inflammation and optimizing hip and pelvis mechanics.
Patient InfoEducation & Resources

Where Our Patients Come From?
Our patients come from all over the United States. We are not limited to serving the southeast. Here is a sample of the regions our patients came from since 2005
Top States
- South Carolina — 2257
- North Carolina — 495
- Georgia — 248
- Florida — 183
- Virginia — 174
International
- Canada — 11
- South America — 7
- The Caribbean — 4
- Europe — 3
- Asia — 1
- Africa — 1
Consultation with Dr. Gross
If you are interested in determining if you are a candidate for surgery, please mail your completed new patient forms to the office and include a digital x-ray. Dr. Gross will call you back to discuss your options.
Consultation with Dr. Browning
If you are interested in a consultation with Dr. Browning, please call ext. 6210 or email. Telehealth visits are available upon request for out-of-state patients.















Today marks the 10th anniversary of my 1st hip resurfacing by Dr Gross. My second will have it’s 10 year anniversary (this year). I can’t believe it’s been 10 years but it’s been an amazing 10 years. Skiing, snowboarding, hiking, golf, travel, sleep have all been made so much better. Heck even wa...